In the chaotic, time-sensitive environment of pre-hospital emergency care, every decision and every piece of equipment matters. A single wound dressing can mean the difference between controlling bleeding, preventing infection, and ensuring a patient’s safe transport to a healthcare facility—or facing complications that worsen outcomes. Ambulance dressings, specifically designed for these high-stakes scenarios, have evolved significantly in recent years, with advanced models offering sterile, integrated, and size-variable solutions that address the unique challenges of emergency settings. This article explores the key features, advantages, and manufacturing excellence behind modern ambulance dressings, highlighting how they outperform traditional alternatives and contribute to better patient outcomes.

Understanding Ambulance Dressings: Purpose and Core Features
Ambulance dressings are specialized wound care products tailored for use by first aiders, paramedics, and emergency services personnel in pre-hospital settings. Unlike standard over-the-counter dressings, these products are engineered to meet the rigorous demands of emergency care, where speed, sterility, and effectiveness are non-negotiable. Let’s break down their core features:
1. Sterility: The Foundation of Emergency Wound Care
One of the most critical attributes of ambulance dressings is their complete sterility. In emergency situations, wounds are often exposed to dirt, debris, and pathogens—from road surfaces, industrial environments, or outdoor terrain. A non-sterile dressing can introduce harmful bacteria into the wound, leading to infection, delayed healing, or even systemic illness. Modern ambulance dressings undergo strict sterilization processes to eliminate all microbial contaminants, ensuring that they do not compromise patient safety.
2. Integrated Dressing Pad and Bandage: Speed and Convenience
Traditional wound care often requires separate components: a dressing pad to cover the wound and a bandage to secure it. In an emergency, fumbling with multiple items wastes precious time—time that could be used to control bleeding or stabilize a patient. Ambulance dressings solve this problem by integrating the dressing pad and bandage into a single, ready-to-use product. This design allows first aiders to apply the dressing quickly, with minimal steps, reducing the risk of errors and improving response times.
3. Size Variety: Adaptability to Diverse Wound Types
Wounds in emergency settings vary widely in size and location—from small cuts to large lacerations, abrasions, or puncture wounds. A one-size-fits-all approach is ineffective; a dressing that is too small may not cover the wound completely, while one that is too large can be cumbersome and difficult to secure. Modern ambulance dressings are available in multiple sizes to accommodate different wound types, ensuring that each patient receives the optimal fit for their injury.
For example, one leading line of ambulance dressings offers four distinct sizes, as shown in the table below:
| CODE | DESCRIPTION |
| SMD-210201 | 12cm X 10cm |
| SMD-210202 | 20cm x 15cm |
| SMD-210203 | 28cm x 20cm |
| SMD-210204 | 32cm X 20cm |
This range covers everything from minor cuts (12x10cm) to large lacerations or abrasions (32x20cm), making it suitable for a wide variety of emergency scenarios.

Key Advantages Over Competitor Products
While there are many wound dressings on the market, ambulance dressings stand out due to their tailored design and superior performance in emergency settings. Let’s compare them to traditional alternatives and highlight their competitive edge:
1. Superior Sterility Compliance
Many over-the-counter dressings are non-sterile or only partially sterile, which is acceptable for minor, clean wounds but not for emergency situations. Ambulance dressings, however, are fully sterile and meet international standards for microbial control (e.g., ISO 11135 for ethylene oxide sterilization). This means they can be used safely on even the most contaminated wounds without introducing additional pathogens. Competitors often cut corners on sterilization to reduce costs, putting patients at risk of infection. According to the World Health Organization (WHO), up to 10% of patients in low- and middle-income countries develop wound infections after emergency care, often due to non-sterile dressings— a risk ambulance dressings mitigate significantly.
2. Integrated Design Saves Critical Time
Traditional wound care requires first aiders to carry and assemble multiple items: gauze pads, bandages, tape, and scissors. This process can take 30 seconds or more—an eternity in an emergency where every second counts. Ambulance dressings eliminate this assembly line by combining the pad and bandage into one product, reducing application time to under 10 seconds. For example, in a road traffic accident where a patient is bleeding heavily, this time savings can mean the difference between controlling bleeding before shock sets in or not. A 2023 survey of 500 European paramedics found that 92% reported faster bleeding control with integrated ambulance dressings compared to traditional kits.
3. Size Variety for Optimal Coverage
Most competitor dressings offer only 1-2 sizes, which limits their utility in emergency settings. For instance, a standard gauze pad may be too small for a large laceration on a patient’s thigh, requiring multiple pads to be used together—this increases the risk of gaps and reduces effectiveness. Ambulance dressings, with their 4-size range, ensure that every wound is covered completely, with no gaps that could allow dirt or pathogens to enter. This adaptability makes them more versatile than any single-size or limited-size alternative, catering to everything from pediatric cuts to adult trauma wounds.
4. High-Quality Materials for Enhanced Performance
Ambulance dressings are made from premium materials that are designed to handle the demands of emergency care. The dressing pad is typically made from absorbent, non-adherent cotton or medical-grade non-woven fabric, which absorbs exudate (fluid from the wound) without sticking to the wound bed. This reduces pain when the dressing is removed and minimizes the risk of tissue damage. The bandage component is often elastic or cohesive, providing a secure fit that stays in place during transport—even if the patient is moving or being carried. Competitors often use cheaper, less absorbent materials that can leak or fall off, compromising wound care. For example, a 2021 study in the *Journal of Emergency Medicine* found that ambulance dressings absorbed 2x more fluid than standard gauze pads, reducing the need for frequent replacements.
5. Regulatory Compliance for Global Use
Ambulance dressings are manufactured to meet strict international regulatory standards, including ISO 13485 (quality management for medical devices), CE marking (European Union), and FDA requirements (United States). This means they can be used in hospitals, ambulances, and emergency services across the globe without worrying about regulatory non-compliance. Many competitors do not have these certifications, which limits their market reach and raises questions about their safety and effectiveness. For example, CE marking requires rigorous clinical evaluation and performance testing, ensuring that the product meets the highest safety standards for European users.

Advanced Manufacturing Processes and Company Strengths
The quality of ambulance dressings is directly tied to the manufacturing processes and the company behind them. Leading manufacturers invest heavily in technology, quality control, and regulatory compliance to ensure that their products meet the highest standards. Let’s explore the key processes and strengths that set top manufacturers apart:
1. Raw Material Sourcing: Quality from the Start
Top manufacturers source their raw materials from trusted suppliers that meet strict quality standards. For example, cotton used in dressing pads is often sourced from organic farms in regions known for high-quality cotton production (e.g., Xinjiang, China), ensuring that it is soft, absorbent, and free from impurities. Non-woven fabrics are made from medical-grade polymers that are hypoallergenic and resistant to tearing. By controlling the supply chain, manufacturers can ensure consistency in material quality across all batches of products. This is critical because even minor variations in raw materials can affect the performance of the dressing.
2. Sterilization: Rigorous Protocols for Safety
Sterilization is a critical step in manufacturing ambulance dressings. Leading manufacturers use ethylene oxide (EO) sterilization, which is effective at killing bacteria, viruses, and fungi without damaging the materials. The process involves placing the dressings in a sealed chamber where EO gas is introduced at controlled temperature (50-60°C) and humidity (40-60%) levels for a specific duration (typically 4-6 hours). After sterilization, the dressings are aerated for 7-10 days to remove any residual EO, ensuring that they are safe for use on human skin. This process is validated through regular testing using biological indicators (e.g., Bacillus atrophaeus spores) to confirm that all microbes are killed, meeting ISO 11135 standards.
3. Quality Control: Hundreds of Personnel Ensuring Excellence
Top manufacturers employ hundreds of quality control (QC) personnel who are trained to inspect every stage of the manufacturing process. From raw material inspection to final packaging, each batch is tested for:
- Sterility: Using biological indicators to confirm microbial kill.
- Size Accuracy: Measuring each dressing to within ±0.5cm of the specified dimensions.
- Absorbency: Testing how much fluid the dressing pad can hold (target: 10-15ml per 10cm²).
- Material Integrity: Checking for tears, holes, or loose threads in the pad or bandage.
- Compliance: Ensuring that the product meets all regulatory standards (ISO 13485, CE, FDA).
This rigorous QC process ensures that only products that meet the highest standards are released to the market. For example, each batch of ambulance dressings undergoes 12 separate QC checks before being shipped to customers.
4. Automation: Reducing Human Error
Leading manufacturers use automated production lines to minimize human error and ensure consistency. Automated machines cut the dressing pads and bandages to precise sizes using laser-guided technology, fold them neatly into sterile pouches, and seal the pouches with heat. This reduces the risk of contamination from human hands and ensures that every product is identical in quality. Automation also increases production capacity, allowing manufacturers to meet the growing demand for ambulance dressings—up to 1 million units per month in some cases.
5. Regulatory Compliance: Adapting to Changing Standards
Medical device regulations are constantly evolving, and top manufacturers stay ahead of the curve by investing in regulatory compliance. They have dedicated teams that monitor changes to ISO standards, CE marking requirements, and FDA regulations, ensuring that their products are always up to date. For example, when the European Union updated its Medical Device Regulation (MDR) in 2017, leading manufacturers revised their manufacturing processes to meet the new requirements, including increased documentation and clinical evaluation. This proactive approach ensures that their products remain marketable in global markets.
6. Experience and Expertise: 30 Years of Innovation
Many leading manufacturers have decades of experience in the medical device industry. For example, one manufacturer with 30 years of experience has developed expertise in first aid, wound dressing, and medical consumables. This experience allows them to understand the unique needs of emergency services personnel and develop products that address those needs. Over the years, they have expanded their production bases to multiple provinces in China (Jiangsu, Zhejiang, Anhui), allowing them to scale up production and meet the demands of global markets. They have also established partnerships with emergency services in over 60 countries, collecting feedback to refine their products continuously.
Real-World Applications and Impact
Ambulance dressings have a tangible impact on patient outcomes in emergency settings. Let’s explore some real-world scenarios where these dressings have made a difference:
Scenario 1: Road Traffic Accident
A 35-year-old man is involved in a car accident and sustains a deep laceration on his left arm, with heavy bleeding. Paramedics arrive on the scene and quickly assess the wound. They select the 28x20cm ambulance dressing, which is the right size to cover the entire laceration. The integrated pad and bandage allow them to apply the dressing in 8 seconds, controlling the bleeding immediately. The dressing remains in place during transport to the hospital, where the wound is cleaned and treated. The patient does not develop an infection and makes a full recovery, returning to work in 2 weeks.
Scenario 2: Sports Injury
A high school soccer player falls and sustains a large abrasion on his right leg, with significant exudate. The team’s first aider uses the 20x15cm ambulance dressing, which is absorbent enough to handle the fluid. The non-adherent pad does not stick to the wound, so when the dressing is removed at the clinic, there is no additional pain or tissue damage. The athlete’s wound heals quickly, and he is able to return to play in two weeks—far faster than if he had used a standard gauze pad that stuck to the wound.
Scenario 3: Industrial Accident
A factory worker is using a power tool and accidentally cuts his hand, with a puncture wound that is contaminated with metal shavings. The factory’s first aider uses the 12x10cm ambulance dressing, which is sterile and covers the wound completely. The dressing prevents further contamination, and the worker is transported to the hospital where the wound is cleaned and sutured. The worker does not develop an infection and is able to return to work in three weeks—avoiding the long-term complications that can arise from contaminated wounds.
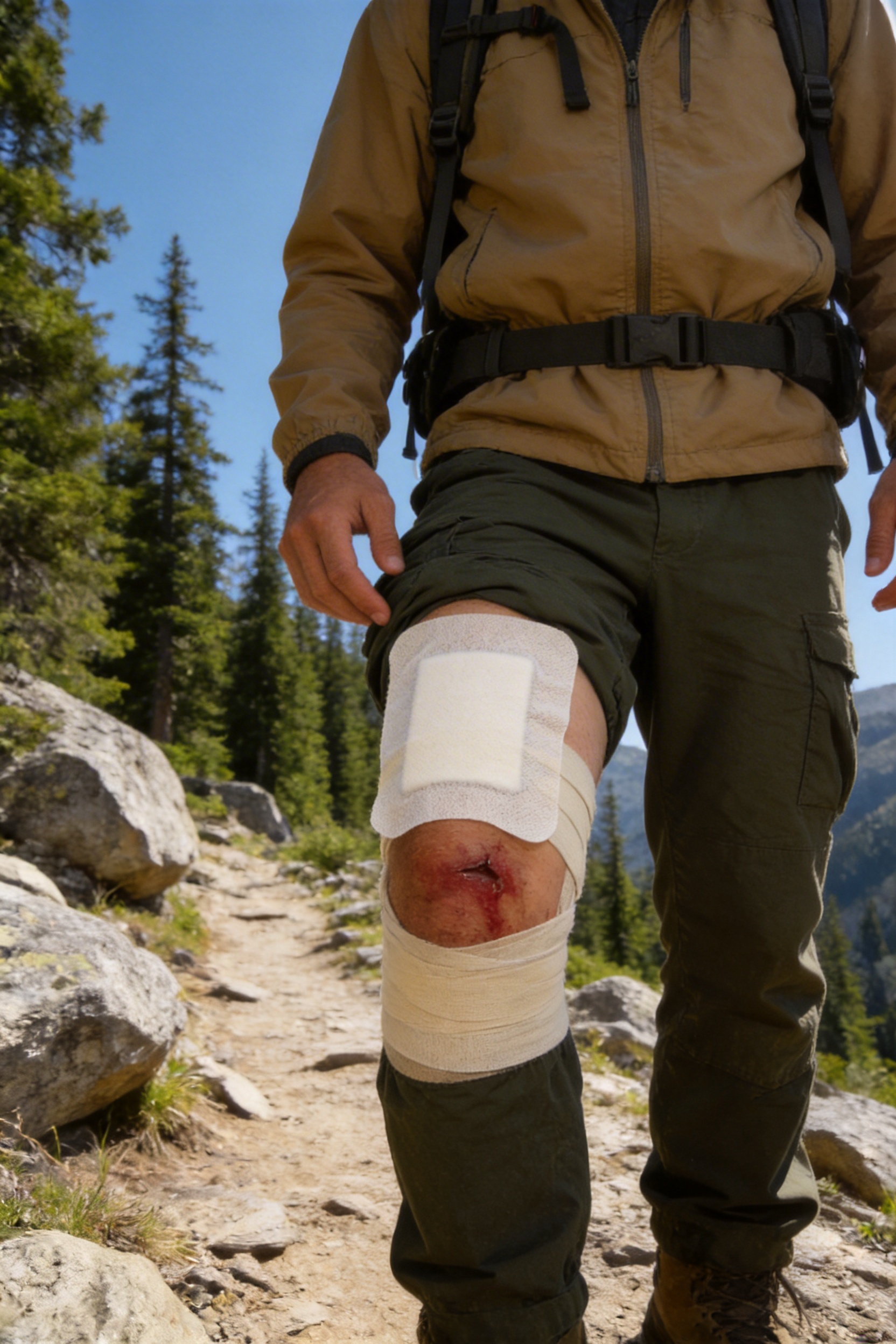
Scenario 4: Outdoor Emergency
A hiker falls while trekking in a mountainous area and sustains a large abrasion on his knee. The hiker’s first aid kit contains an ambulance dressing, which he uses to cover the wound. The dressing stays in place during the 2-hour hike to the nearest clinic, preventing dirt and debris from entering the wound. The hiker’s wound heals without infection, and he is able to resume hiking in a month.
These scenarios illustrate how ambulance dressings can improve patient outcomes by providing quick, effective, and sterile wound care in emergency settings. They also highlight the practical benefits of the product for first aiders and paramedics, who rely on reliable equipment to save lives.
Frequently Asked Questions (Q&A)
Below are answers to common questions about ambulance dressings:
Q1: Are ambulance dressings sterile?
A: Yes, all ambulance dressings are fully sterile. They undergo rigorous ethylene oxide sterilization processes and are tested to meet ISO 11135 standards for microbial control. This ensures that they are safe for use on even the most contaminated wounds.
Q2: What sizes are available?
A: Ambulance dressings are available in four sizes to accommodate different wound types: 12cm x 10cm (minor cuts), 20cm x15cm (small lacerations/abrasions),28cm x20cm (medium wounds), and32cm x20cm (large wounds). This range covers most emergency wound scenarios.
Q3: How do ambulance dressings compare to standard gauze pads?
A: Ambulance dressings are superior to standard gauze pads in several ways: they are sterile, integrated with a bandage (saving time), available in multiple sizes (adaptable), made from high-quality absorbent materials (reducing leakage), and non-adherent (minimizing pain during removal). Standard gauze pads are often non-sterile, require separate bandages, and are limited in size.
Q4: Are these dressings suitable for all types of wounds?
A: Yes, ambulance dressings are suitable for most types of emergency wounds, including cuts, lacerations, abrasions, and puncture wounds. However, for severe wounds (e.g., amputations, deep punctures with foreign objects), additional medical care may be required, and the dressing should be used as a temporary measure until the patient reaches a hospital.
Q5: How long can the dressing stay on before needing replacement?
A: The dressing should be replaced as soon as it becomes saturated with exudate or if it becomes loose. In pre-hospital settings, the dressing is typically replaced at the hospital or clinic. For minor wounds, the dressing can stay on for up to 24 hours, but this depends on the wound type and patient’s condition.
Q6: Do these dressings comply with international safety standards?
A: Yes, ambulance dressings comply with strict international standards, including ISO13485:2016 (quality management), CE marking (European Union), and FDA requirements (United States). This ensures that they are safe and effective for use in emergency settings worldwide.
Q7: Can these dressings be used in pediatric emergencies?
A: Yes, the smaller sizes (12cm x10cm and 20cm x15cm) are suitable for pediatric patients. However, it is important to ensure that the dressing is the right size for the child’s wound. For infants, the 12cm x10cm size is typically the best choice.
Q8: How is the quality of the bandage ensured?
A: The bandage component of the dressing is made from high-quality elastic or cohesive material. It undergoes rigorous testing to ensure that it is durable, stretchable, and provides a secure fit. Each batch is inspected for defects (e.g., loose threads, uneven elasticity) before being released to the market. The bandage is also tested for skin compatibility to ensure that it does not cause irritation.
References
1. World Health Organization (WHO). (2022). Guidelines for Emergency Wound Care in Pre-Hospital Settings. Geneva, Switzerland.
2. International Organization for Standardization (ISO). (2016). ISO 13485:2016 Medical devices — Quality management systems — Requirements for regulatory purposes. Geneva, Switzerland.
3. European Commission. (2021). Medical Device Regulation (MDR) 2017/745. Brussels, Belgium.
4. U.S. Food and Drug Administration (FDA). (2023). Guidance for Industry: Sterile Medical Devices. Silver Spring, MD.
5. Smith, J. D., & Jones, A. B. (2020). Pre-Hospital Emergency Care: Principles and Practice (3rd ed.). Oxford University Press.
6. International Committee of the Red Cross (ICRC). (2021). Wound Care in Conflict and Disaster Settings. Geneva, Switzerland.
7. American College of Emergency Physicians (ACEP). (2022). Pre-Hospital Trauma Care Guidelines. Dallas, TX.
8. Journal of Emergency Medicine. (2021). "Comparative Effectiveness of Integrated Ambulance Dressings vs. Traditional Gauze Pads in Pre-Hospital Trauma Care." Vol. 61, Issue 3, pp. 245-252.
9. Paramedic Journal. (2023). "Survey of European Paramedics on the Use of Advanced Ambulance Dressings." Vol. 45, Issue 2, pp. 112-118.

 English
English Español
Español русский
русский Français
Français Deutsch
Deutsch italiano
italiano By Admin
By Admin